Breast implant-assocaited anaplastic large cell lymphoma (BIA-ALCL) latest news
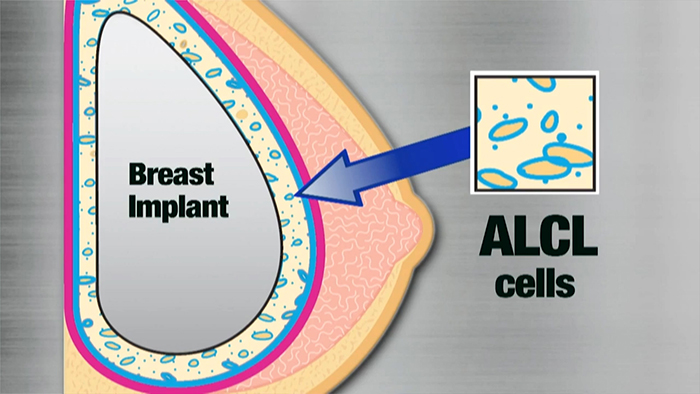
Breast implant-associated anaplastic large cell lymphoma (BIA-ALCL) is an uncommon and highly treatable type of lymphoma that can develop around breast implants. BIA-ALCL occurs most frequently in patients who have breast implants with textured surfaces. The current lifetime risk of BIA-ALCL is estimated to be 1:3817 - 1:30,000 women with textured implants based upon current confirmed cases and textured implant sales data over the past two decades. Since the initial case report in 1996, ASPS now recognizes approximately 274 cases in the US and a total of 694 worldwide as of April 19, 2019.
Most of the patients who have developed BIA-ALCL receive an excellent prognosis following surgical removal of the breast implants and the surrounding scar tissue capsule. Continued follow-up after any breast implant surgery is suggested and important for patient health, but patients who notice pain, lumps, swelling, fluid collections or unexpected changes in breast shape, including asymmetry, should contact their plastic surgeon. In most cases, women diagnosed with BIA-ALCL observed changes in the look or feel of the area surrounding the implant greater than one year after their initial surgical sites were fully healed, and on average eight to ten years after receiving textured implants.
Patients undergoing plastic surgery procedures, aesthetic or reconstructive, should be thoroughly informed of the potential risks and possible complications known to be associated with the procedure, and any device used in that procedure. In the very rare cases where a diagnosis of BIA-ALCL is made, surgical treatment is essential for the management of the disease. Some patients with more advanced disease may require further treatment such as chemotherapy.
FDA updates on BIA-ALCL
The February 6, 2019 FDA website update acknowledges that while it remains difficult to determine the exact number of BIA-ALCL cases, there have now been 660 medical device reports (MDR) reported to the FDA Manufacturer and User Facility Device Experience (MAUDE) database as of September 30, 2018, and after thorough review, the FDA reports 457 unique cases meeting pathology criteria for BIA-ALCL. Of these MDRs, included data related to the implant surface, with 24 identified as smooth, majority of these demonstrate a clinical history of a textured device in the clinical history. The update also confirms that both silicone gel and saline implants have been reported in cases of BIA-ALCL.
It's important to note that the FDA acknowledges that the MAUDE database may contain limited and potentially inaccurate adverse event reports, and may not represent the true number of U.S. cases, as some entries are duplicates and not all cases are confirmed as ALCL. Though the FDA indicated it has received 24 reports associated with smooth implants including some smooth surface-only cases of BIA-ALCL reported, they acknowledge that this information is "unverified" and potentially "inaccurate." As of April 19, 2019, 274 suspected/confirmed U.S. cases of BIA-ALCL have been reported to the Patient Registry and Outcomes For breast Implants and anaplastic large cell Lymphoma Etiology and Epidemiology (PROFILE) Registry, a joint collaboration between ASPS, PSF and the FDA.
The FDA's website update confirms previous ASPS communications, noting that BIA-ALCL remains a rare condition that occurs most frequently in patients who have breast implants with textured surfaces. The report also reiterates that patients should discuss with their health-care provider the benefits and risks of textured-surface versus smooth-surface implants. The FDA highlights the World Health Organization recognition of BIA-ALCL, and standardized diagnosis and treatment guidelines established by the National Comprehensive Cancer Network (NCCN).
The FDA recommends that all cases of BIA-ALCL be reported to the FDA and to the PROFILE registry.
For more information on BIA-ALCL, visit plasticsurgery.org/alcl or the FDA website.
Our practice is committed to patient safety, advancing quality of care, and practicing medicine based upon the best available scientific evidence. We will continue to monitor and review all new information as it becomes available to keep the plastic surgery community informed.
Source: American Society of Plastic Surgery

